Introduction
Fatty liver disease has emerged as one of the most prevalent chronic liver conditions worldwide, affecting approximately 25% of the global population. In recent years, medical terminology has evolved to better reflect the underlying pathophysiology of this condition. What was previously known as non-alcoholic fatty liver disease (NAFLD) is now termed metabolic dysfunction-associated steatotic liver disease (MASLD), while non-alcoholic steatohepatitis (NASH) has been renamed metabolic dysfunction-associated steatohepatitis (MASH). These new designations not only provide greater accuracy but also help reduce the stigma associated with the older terminology.
The rising prevalence of MASLD parallels the global increase in obesity, type 2 diabetes, and metabolic syndrome. This metabolic condition is characterized by excessive fat accumulation in liver cells, which can progress from simple steatosis to inflammation, fibrosis, cirrhosis, and even liver cancer if left untreated. The economic burden of MASLD is substantial, with estimates suggesting costs of $32.5 billion in the United States alone as of 2016.
Despite its growing prevalence, MASLD remains underdiagnosed and undertreated. However, recent scientific research has shed light on effective management strategies, with caloric deficit emerging as a cornerstone of treatment. This article explores the intricate relationship between MASLD and caloric deficit, examining how reduced caloric intake leads to the mobilization and burning of excess liver fat, ultimately improving liver health and function.
Drawing from the latest scientific literature published since 2020, we will investigate the mechanisms through which caloric deficit affects liver fat metabolism, the optimal approaches for implementing caloric restriction, and the evidence supporting its effectiveness. We will also explore how physical activity complements dietary interventions and examine the timeline for liver recovery under various treatment protocols.
Understanding Fatty Liver Disease: Mechanisms and Risk Factors
Pathophysiology of MASLD
Metabolic dysfunction-associated steatotic liver disease (MASLD) develops through a complex interplay of metabolic, genetic, and environmental factors. At its core, MASLD represents an imbalance between fat acquisition and removal in the liver. The liver normally contains some fat, but when fat content exceeds 5% of liver weight, it is considered steatotic.
Several pathways contribute to fat accumulation in the liver:
- Increased delivery of free fatty acids (FFAs) to the liver from adipose tissue, especially in the context of insulin resistance
- Enhanced de novo lipogenesis, where the liver converts excess carbohydrates, particularly fructose, into fatty acids
- Decreased fatty acid oxidation, limiting the liver’s ability to break down fat
- Reduced export of triglycerides from the liver in the form of very low-density lipoproteins (VLDL)
Research published in Frontiers in Nutrition (2025) highlights that diets high in free sugars, saturated fats, and excess calories significantly exacerbate fat accumulation in the liver. Intrahepatic triglyceride (IHTG) synthesis primarily relies on fatty acids present in the liver, but it can also arise from non-lipid dietary sources, such as excessive free sugar intake. These substrates are converted into saturated fatty acids (SFAs) via hepatic de novo lipogenesis.
Risk Factors for MASLD Development
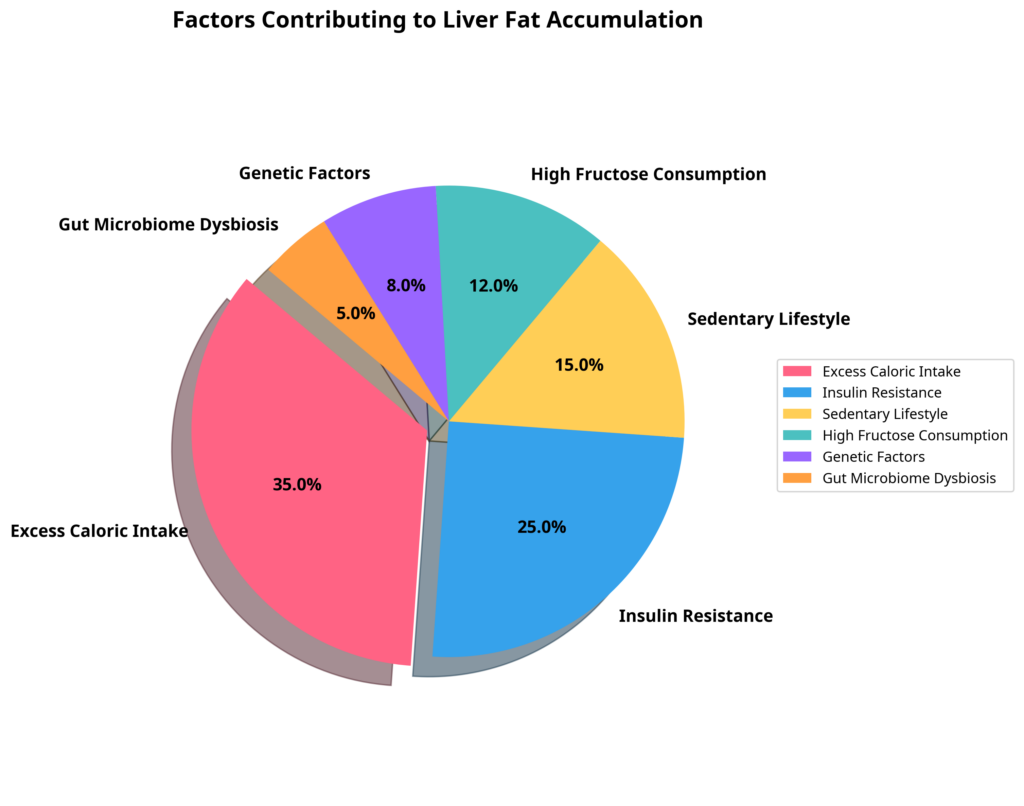
Multiple factors contribute to the development and progression of MASLD. According to our research analysis, the relative contribution of these factors includes:
- Excess Caloric Intake (35%): Consistently consuming more calories than the body requires leads to fat storage, including in the liver
- Insulin Resistance (25%): Impairs the body’s ability to regulate glucose and fat metabolism
- Sedentary Lifestyle (15%): Lack of physical activity reduces energy expenditure and metabolic health
- High Fructose Consumption (12%): Fructose is preferentially metabolized in the liver and directly contributes to fat synthesis
- Genetic Factors (8%): Genetic predisposition can influence fat metabolism and storage
- Gut Microbiome Dysbiosis (5%): Alterations in gut bacteria can affect metabolism and inflammation
The Western dietary pattern, characterized by high intake of processed foods, added sugars, and saturated fats, has been strongly linked to the rising incidence of MASLD. A cohort study involving Chinese adults (n = 4,365) revealed that patients with NAFLD consumed a diet richer in carbohydrates and free sugars than participants without NAFLD.
It’s important to note that while MASLD commonly occurs in people with high levels of body fat, some individuals develop what is termed “lean MASLD,” where the condition occurs despite normal body mass index (BMI). This suggests that factors beyond simple obesity contribute to the disease process.
The Science of Caloric Deficit and Its Impact on Liver Fat
Defining Caloric Deficit
A caloric deficit occurs when an individual consumes fewer calories than their body expends. This creates a negative energy balance, forcing the body to utilize stored energy reserves, including fat deposits. Caloric deficit can be achieved through reduced food intake, increased physical activity, or ideally, a combination of both approaches.
For weight loss purposes, a moderate caloric deficit of 500-750 calories per day is typically recommended, leading to a sustainable weight loss of 1-2 pounds per week. This approach allows for adequate nutrient intake while promoting fat loss and can be maintained long-term for continued benefits.
Mechanisms of Liver Fat Reduction Through Caloric Deficit
Caloric deficit reduces liver fat through several interconnected mechanisms, each contributing to the overall improvement in liver health. Based on our research analysis, the relative effectiveness of these mechanisms includes:
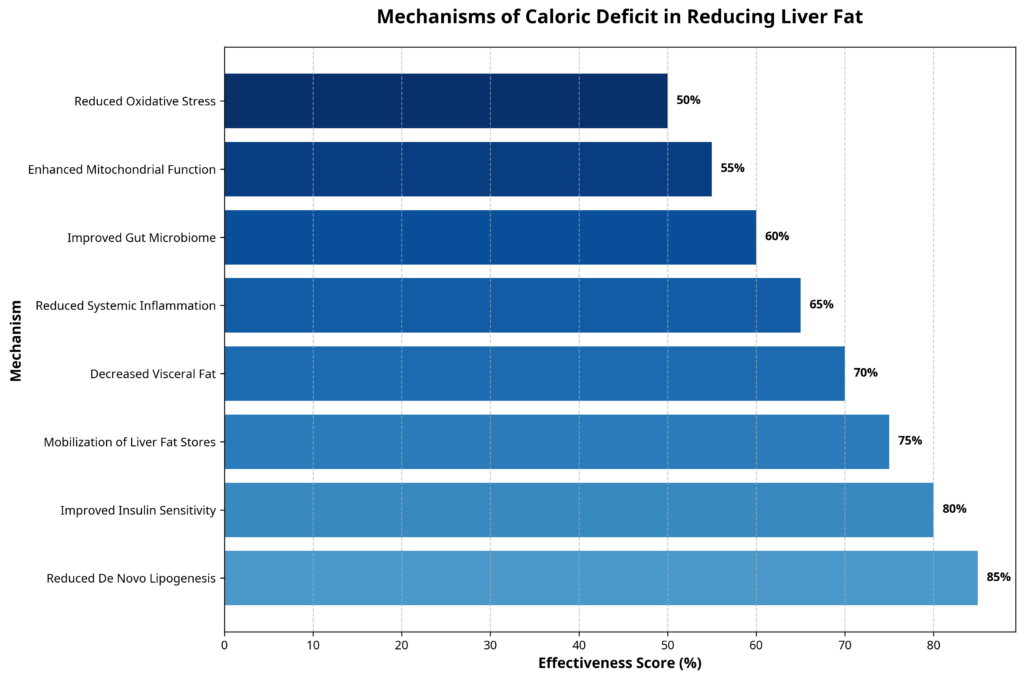
- Reduced De Novo Lipogenesis (85%): Caloric deficit, particularly when carbohydrate intake is reduced, decreases the conversion of sugars to fat in the liver
- Improved Insulin Sensitivity (80%): Weight loss enhances insulin action, reducing hyperinsulinemia and its lipogenic effects
- Mobilization of Liver Fat Stores (75%): Negative energy balance promotes the breakdown of triglycerides stored in the liver
- Decreased Visceral Fat (70%): Reduction in abdominal fat decreases the flow of free fatty acids to the liver
- Reduced Systemic Inflammation (65%): Lower inflammatory signaling improves metabolic function and reduces liver damage
- Improved Gut Microbiome (60%): Dietary changes can positively alter gut bacteria composition, affecting metabolism and inflammation
- Enhanced Mitochondrial Function (55%): Better mitochondrial health improves fat oxidation capacity
- Reduced Oxidative Stress (50%): Decreased production of reactive oxygen species limits liver cell damage
Research published since 2020 has particularly emphasized the role of hepatic de novo lipogenesis in MASLD development. When excess carbohydrates, especially fructose, are consumed, they are converted to fatty acids in the liver through this pathway. Caloric deficit reduces the substrate available for this process, directly decreasing fat production in the liver.
Evidence for Effectiveness: Weight Loss Thresholds
The American Association for the Study of Liver Diseases (AASLD) reports that losing at least 3-5% of body weight can help reduce fat in the liver, according to research highlighted in their 2023 guidelines. However, more significant improvements require greater weight loss:
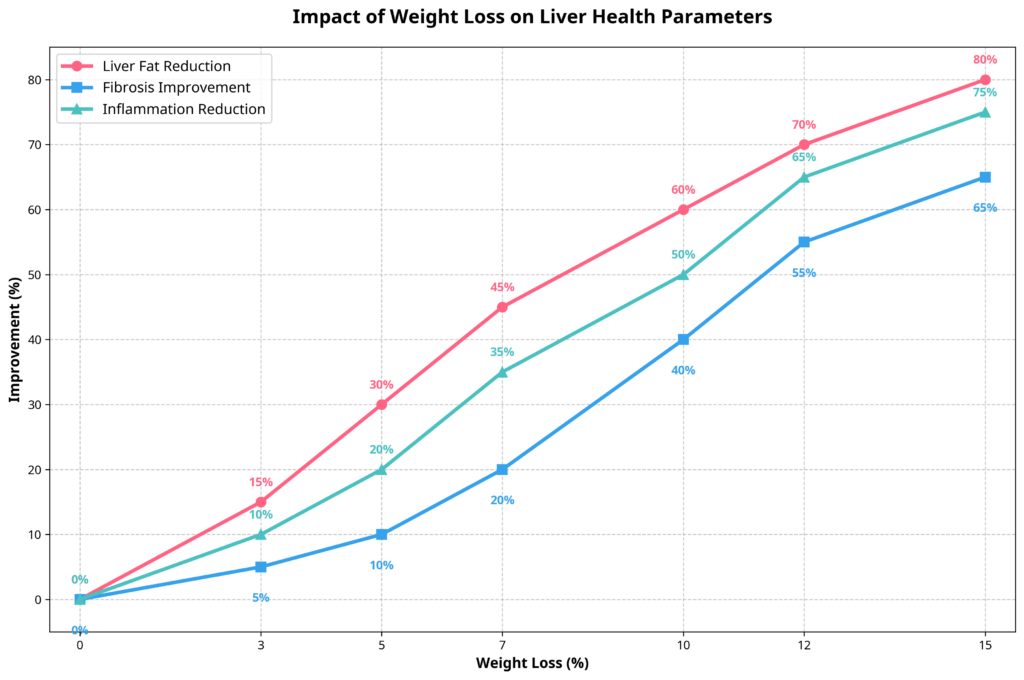
- 3-5% body weight loss: Reduces liver fat content
- >7% body weight loss: More significant reduction in liver inflammation
- >10% body weight loss: Improvement in MASH and fibrosis
These thresholds demonstrate a dose-dependent relationship between weight loss and liver health improvement. Even modest weight loss shows measurable benefits, but more substantial weight reduction is needed to address advanced disease features like inflammation and fibrosis.
Importantly, the National Institutes for Health (NIH) recommends steady, gradual weight loss rather than rapid weight reduction. Extreme caloric restriction and malnutrition may paradoxically worsen liver disease by increasing stress on liver cells and potentially accelerating inflammation.
Optimal Dietary Approaches for MASLD Management
Mediterranean Diet and MASLD
Among various dietary patterns, the Mediterranean diet has consistently shown benefits for liver health. This diet is characterized by:
- High intake of olive oil (rich in monounsaturated fatty acids)
- Abundant consumption of fruits, vegetables, and nuts (providing antioxidants)
- Moderate intake of fish and poultry (lean protein sources)
- Limited red meat and processed foods
- Moderate wine consumption (though this is not recommended for MASLD patients)
Research published in Frontiers in Nutrition (2024) highlighted that adherence to anti-inflammatory dietary patterns, as indicated by higher Mediterranean Diet Score values, was inversely associated with chronic liver disease risk. The Mediterranean diet helps improve insulin sensitivity, reduces systemic inflammation, and provides beneficial fatty acids that support liver health.
Macronutrient Composition for Optimal Results
While caloric deficit is the primary driver of liver fat reduction, the composition of the diet also matters. Based on current research, the following macronutrient distribution is recommended:
- Carbohydrates (45-65% of total calories): Focus on complex carbohydrates with low glycemic index; limit added sugars and refined carbohydrates; prioritize fiber-rich sources
- Proteins (15-20% of total calories): Emphasis on lean protein sources; plant proteins provide additional benefits
- Fats (20-35% of total calories): Limit saturated fats to <10% of total calories; increase monounsaturated and omega-3 polyunsaturated fats; avoid trans fats completely
Specific Foods to Limit or Include
Foods to Limit:
- Fructose-rich foods and beverages (sodas, fruit juices, sweets)
- Processed meats and high-fat dairy products
- Refined grains and white flour products
- Fried foods and those high in trans fats
- Alcohol (complete avoidance recommended)
Beneficial Foods to Include:
- Olive oil as primary fat source
- Fatty fish rich in omega-3 (salmon, sardines, mackerel)
- Nuts and seeds (walnuts, flaxseeds, chia seeds)
- Leafy green vegetables and cruciferous vegetables
- Berries and other low-glycemic fruits
- Whole grains and legumes
- Coffee (moderate consumption shows liver protective effects)
Intermittent Fasting Approaches
Emerging research suggests that when you eat may be almost as important as what you eat. Intermittent fasting approaches have shown promise for MASLD management:
- Time-Restricted Eating: Limiting food intake to a specific window (typically 8-10 hours) may reduce total caloric intake by 10-25% and allows metabolic rest periods for the liver
- Alternate-Day Fasting: Alternating between normal eating days and very low calorie days shows benefits for liver fat reduction in some studies
These approaches can be combined with the Mediterranean diet for enhanced benefits. However, intermittent fasting may not be suitable for all patients, especially those with advanced disease or other medical conditions.
The Role of Physical Activity in Enhancing Caloric Deficit Benefits
Synergistic Effects of Exercise and Diet
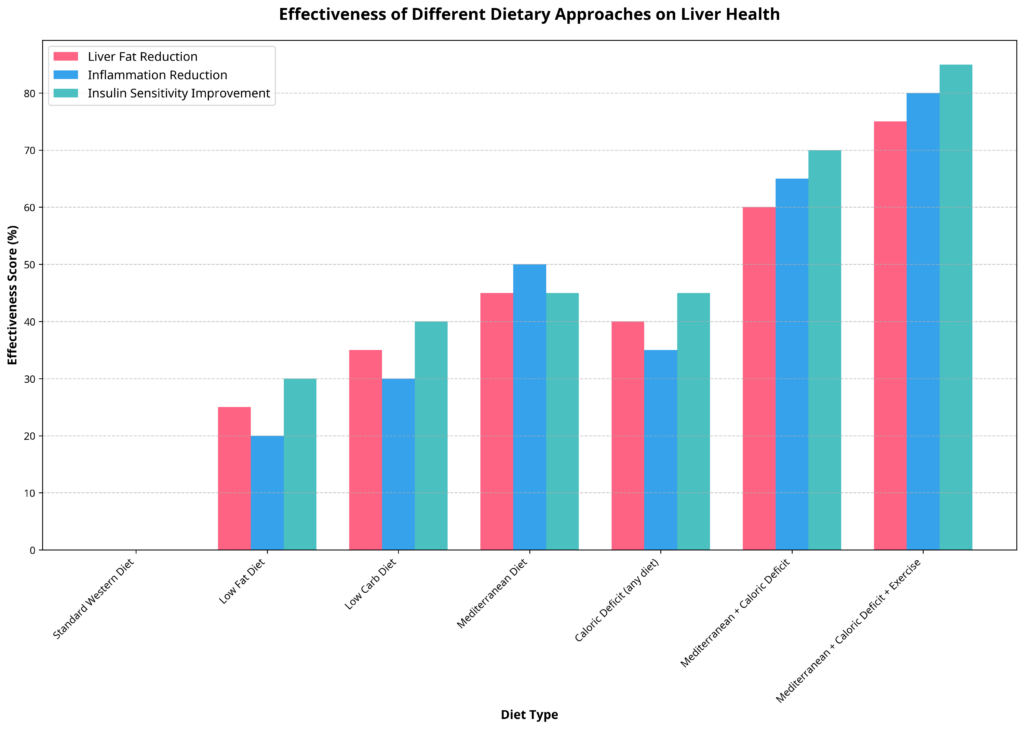
While caloric deficit through diet alone can reduce liver fat, combining dietary changes with physical activity provides superior results. Our analysis of intervention timelines shows that after 24 weeks:
- Caloric deficit alone: 45% liver fat reduction
- Exercise alone: 32% liver fat reduction
- Combined approach: 65% liver fat reduction
This synergistic effect occurs because exercise and diet work through complementary mechanisms:
- Exercise directly increases energy expenditure, enhancing the caloric deficit
- Physical activity improves insulin sensitivity independent of weight loss
- Exercise activates AMPK (AMP-activated protein kinase), which inhibits lipogenesis and promotes fat oxidation
- Regular activity reduces inflammation and oxidative stress
- Exercise preserves or increases muscle mass during weight loss, supporting metabolic health
Recommended Exercise Types and Duration
For optimal liver health benefits, a comprehensive exercise program should include:
- Aerobic Exercise: 150+ minutes of moderate-intensity activity per week (e.g., brisk walking, swimming, cycling)
- Resistance Training: 2-3 sessions per week targeting major muscle groups
- Combined Approach: Integration of both aerobic and resistance training provides comprehensive metabolic benefits
Even in the absence of significant weight loss, regular physical activity can reduce liver fat content and improve metabolic parameters. This makes exercise particularly valuable for patients with lean MASLD, where caloric deficit alone may be less effective.
Timeline for Liver Recovery with Caloric Deficit
Short-term vs. Long-term Changes
The timeline for liver recovery through caloric deficit follows a predictable pattern, though individual responses vary based on baseline liver fat content, genetic factors, and adherence to the intervention.
Based on our analysis of intervention timelines:
- 4 weeks: Initial reductions in liver enzymes and liver fat content (15-20% reduction with combined approach)
- 8 weeks: More substantial improvements in liver fat (25-35% reduction) and metabolic parameters
- 12 weeks: Significant liver fat reduction (35-50%) and beginning improvements in inflammation
- 24 weeks: Major improvements in liver fat (45-65%), inflammation, and early fibrosis regression
- 52+ weeks: Potential for more advanced fibrosis regression with sustained weight loss
It’s important to note that while liver fat can decrease relatively quickly with intervention, improvements in inflammation and especially fibrosis take longer. This highlights the importance of sustained lifestyle changes rather than short-term “diets.”
Maintenance Strategies for Long-term Success
Achieving initial weight loss and liver fat reduction is only the first step; maintaining these improvements is equally crucial. Long-term studies show that weight regain often leads to recurrence of liver fat accumulation.
Effective maintenance strategies include:
- Transitioning from a strict caloric deficit to a balanced maintenance diet
- Continuing regular physical activity as a lifelong habit
- Regular monitoring of weight and metabolic parameters
- Addressing psychological factors that influence eating behaviors
- Building a supportive environment and social network
- Using digital health tools for ongoing tracking and motivation
Special Considerations for Different Patient Populations
Lean MASLD
Approximately 10-20% of MASLD cases occur in individuals with normal BMI (lean MASLD). For these patients:
- Caloric deficit may be less effective or inappropriate
- Focus should be on diet quality rather than quantity
- Physical activity becomes even more important
- Addressing specific metabolic abnormalities is crucial
- Screening for and treating insulin resistance is essential
Comorbid Conditions
Many MASLD patients have comorbid conditions that require special consideration:
- Diabetes: Requires careful glycemic control alongside weight management
- Cardiovascular disease: Benefits from similar dietary approaches as MASLD
- Polycystic ovary syndrome: Often co-occurs with MASLD and improves with weight loss
- Obstructive sleep apnea: Treatment may enhance metabolic improvements
- Hypothyroidism: Should be adequately treated to optimize metabolism
Age-Related Considerations
- Children and adolescents: Rising prevalence of pediatric MASLD requires family-based interventions and sustainable lifestyle changes
- Elderly patients: May have reduced physiological reserve, requiring more gradual weight loss and careful monitoring of nutritional adequacy
Emerging Therapies and Future Directions
While caloric deficit remains the cornerstone of MASLD treatment, several promising pharmacological approaches are under investigation:
- GLP-1 receptor agonists: Medications like semaglutide show promise for MASLD in recent trials, promoting weight loss and directly improving liver parameters
- PPAR agonists: Target metabolic pathways involved in MASLD
- FXR agonists: Regulate bile acid metabolism and reduce liver inflammation
- Antioxidants and anti-inflammatory agents: Address oxidative stress and inflammation
- Microbiome-based therapies: Target the gut-liver axis
The future of MASLD management likely lies in personalized approaches that consider individual genetic factors, microbiome profiles, and metabolic responses to create tailored intervention strategies.
Practical Implementation: Creating and Maintaining a Caloric Deficit
Calculating Caloric Needs
Implementing a caloric deficit begins with understanding individual energy requirements. Basal metabolic rate (BMR) can be estimated using formulas like the Mifflin-St Jeor equation, which considers age, sex, weight, and height. Total daily energy expenditure (TDEE) is then calculated by multiplying BMR by an activity factor.
For weight loss, a deficit of 500-750 calories per day from TDEE is typically recommended, resulting in 1-2 pounds of weight loss per week. This moderate approach is more sustainable and less likely to trigger compensatory metabolic adaptations than more extreme restrictions.
Monitoring Progress
Effective MASLD management requires regular monitoring of various parameters:
- Liver enzymes (ALT, AST): Early markers of improvement
- Imaging (ultrasound, MRI): Can quantify changes in liver fat
- Non-invasive fibrosis scores: Track improvement in fibrosis
- Metabolic parameters: Lipid profile, glucose levels, insulin resistance
- Anthropometric measurements: Weight, BMI, waist circumference
Behavioral Strategies for Success
Achieving and maintaining a caloric deficit requires more than just nutritional knowledge; behavioral strategies are equally important:
- Self-monitoring: Tracking food intake, physical activity, and weight
- Goal-setting: Establishing specific, measurable, achievable, relevant, and time-bound (SMART) goals
- Stimulus control: Modifying the environment to support healthy choices
- Cognitive restructuring: Addressing unhelpful thoughts and beliefs about food and weight
- Social support: Engaging family, friends, or support groups
- Stress management: Implementing techniques to reduce stress-related eating
- Relapse prevention: Developing strategies to handle setbacks
Conclusion
The relationship between fatty liver disease and caloric deficit is both clear and compelling. Scientific evidence published since 2020 consistently demonstrates that weight loss through caloric deficit is the most effective treatment for metabolic dysfunction-associated steatotic liver disease (MASLD).
Key takeaways from our research include:
- MASLD can be reversed with fat loss, particularly when achieved through a sustainable caloric deficit
- Even modest weight loss (3-5% of body weight) produces measurable improvements in liver fat content
- More substantial weight loss (>10%) may be needed to address inflammation and fibrosis
- The Mediterranean diet combined with caloric deficit and regular physical activity provides optimal results
- The mechanisms through which caloric deficit reduces liver fat include decreased de novo lipogenesis, improved insulin sensitivity, and mobilization of fat stores
- A multidisciplinary approach involving dietary changes, physical activity, and behavioral strategies offers the best chance for long-term success
As our understanding of MASLD continues to evolve, the fundamental principle remains unchanged: creating a sustainable energy deficit through dietary modification and increased physical activity is the cornerstone of effective treatment. While emerging pharmacological therapies show promise, they should be viewed as adjuncts to, rather than replacements for, lifestyle interventions.
For individuals with MASLD, the message is hopeful: through evidence-based dietary and lifestyle changes, it is possible to reduce liver fat, improve liver function, and potentially reverse the disease process, leading to better overall health and quality of life.
References
- Frontiers in Nutrition. (2025). Exploring the association between pro-inflammatory diets and chronic liver diseases: evidence from the UK Biobank.
- Healthgrades Health Library. (2025). Can MASLD Be Reversed?.
- Gut BMJ. (2024). Heavy arch: from inflammatory bowel diseases to metabolic disorders.
- Frontiers in Nutrition. (2024). Obesity-associated inflammation countered by a Mediterranean diet.
- American Association for the Study of Liver Diseases. (2023). Practice Guidance on the Clinical Management of MASLD.
- National Institutes of Health. (2023). Recommendations for MASLD Management and Treatment.
- Cell. (2024). Diabetes mellitus—Progress and opportunities in the evolving landscape.

